A Vancouver-based infectious diseases specialist says people shouldn't always stay home if they feel ill — sometimes a visit to the hospital could mean the difference between life and death.
While they are extremely rare, infections from bacteria that cause flesh-eating diseases are on the rise across British Columbia.
Strep A infections typically cause mild illnesses such as strep throat or skin rashes and most people recover with antibiotics.
However, when the infection becomes invasive (and becomes iGAS), it can cause life-threatening pneumonia, sepsis, toxic shock syndrome and necrotizing fasciitis, also known as flesh-eating disease.
"But the vast majority of these infections are benign," Dr. Brian Conway, medical director of the Vancouver Infectious Diseases Centre (VIDC), told V.I.A. "Ninety-five to 99 per cent of infections [are benign]."
The uptick in strep A infections has also been felt across the world, with countries on multiple continents reporting an increase in cases.
A Vancouver firefighter recently travelled to Hong Kong with his partner and developed flesh-eating disease from a strep A infection, forcing the amputation of his leg.
How do you get flesh-eating disease?
Strep A is a bacterial disease that is spread from person to person by nose and mouth secretions from an infected individual.
Some of the ways the disease spreads are through:
- Breathing in air contaminated with streptococcal bacteria when an infected person has coughed, sneezed, or talked
- Kissing, sharing drinking cups, forks, spoons, or cigarettes
- Touching the nose and throat secretions of an infected person
- Touching articles recently contaminated with the nose and throat secretions of an infected person
People with chronic illnesses such as cancer, diabetes, and chronic heart or lung disease, and those who use medications such as steroids have a higher risk for contracting strep A. People with an open wound, a cut, or chicken pox, who have a history of alcohol abuse or injection drug use, also have a higher risk for disease. Elderly people may also be more susceptible to infection.
What are the symptoms of flesh-eating disease?
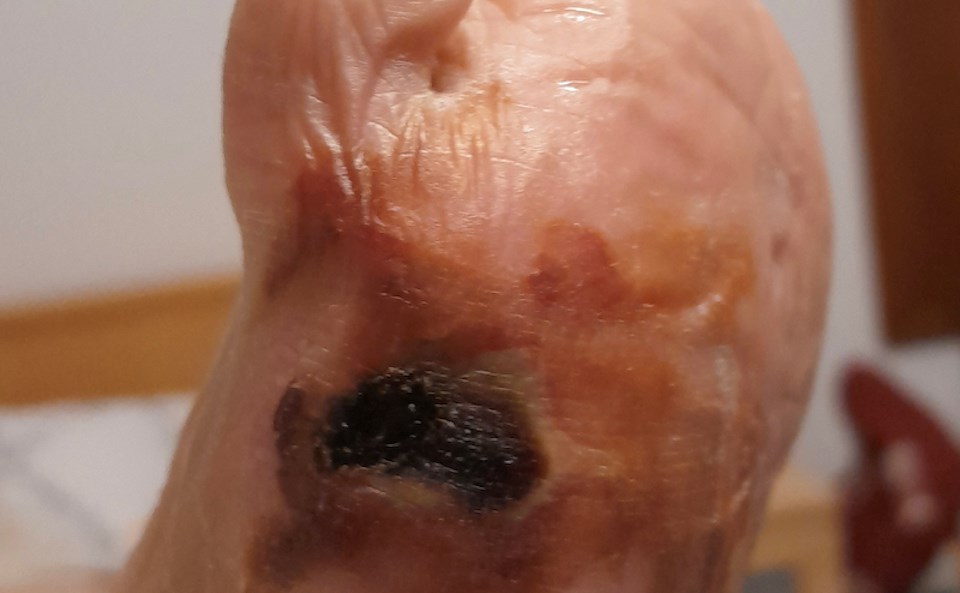
While flesh-eating disease rapidly develops and can be fatal, the infection may start with a small red rash and fever, which may seem somewhat benign. Over the pandemic, British Columbians were encouraged to stay home if they could manage their symptoms at home.
But anyone who has severe pain and swelling, a fever, and redness around a wound should seek emergency care.
"This is a rapidly progressing illness," Conway emphasized. "There is no incubation period."
People who experience rapidly spreading, "significant pain" as the infection worsens should consult a health-care professional immediately. While a doctor may prescribe antibiotics, surgery may be required if the bacteria has spread.
"If they have a severe throat infection and shortness of breath, [the individual] may need to go to the emergency room," he explained.
The tissue in the affected area can quickly die from a lack of blood supply. However, the chances of getting necrotizing fasciitis caused by strep A are very low. In B.C., about four people out of 1 million get it every year.
What other infections can strep A cause?
Strep A can also streptococcal toxic shock syndrome, which can be fatal.
According to the BC Centre for Disease Control (BCCDC), symptoms of toxic shock include:
- fever
- sudden severe pain, often in an arm or leg
- dizziness
- confusion
- feelings of having “the flu"
- a flat red rash over large areas of the body.
Strep A can also cause septicemia (blood poisoning).
Septicemia symptoms include:
- fever
- chills
- headache
- generally not feeling well
- pale skin
- lack of energy
- rapid breathing
- increased heart rate.
Why do only some people develop severe symptoms from strep A?
Conway says there is "no clear biological explanation" why some people get severe infections from strep A. People can have a "completely normal" and healthy immune system and still have life-threatening complications.
"To some extent, it might be the wrong person at the wrong place at the wrong time," he said. "We need to emphasize how rare this is but in some cases, the consequences can be catastrophic leading up to death."
Different kinds of bacteria can also cause a similar clinical disease. This happens more often in people who have weakened immune systems or who are diabetic.
A person can also have COVID-19 and strep throat concurrently because it is easier to contract another illness with an already weakened immune system.
Conway highlights that former Quebec Premier Lucien Bouchard suffered from a flesh-eating disease in 1994, resulting in the amputation of his left leg.
"This also isn't something completely new that is just sneaking up on us. It has been around for decades."
But anyone who has a severe throat infection, or who feels very unwell in a short period of time, should seek medical attention.
"It is correct to say that over the past year, there has been an uptick in the number of severe group A strep infections and the mortality associated with them," he cautioned.
"We are still trying to understand this [and you may have] a very serious condition.
"If you think you should go [to the hospital], you should go."
With files from Graeme Wood